Like many people these days, I often spend part of my evenings watching some of the excellent series and miniseries currently available on cable TV. Recently, I noticed an interesting trend. I was watching three different shows, jumping from one to another on different evenings just for a change of pace. The shows in question were Poldark, Homecoming and Maniac. Poldark is a long running series about romantic events taking place in late 18th century Cornwall, whereas both Homecoming and Maniac are, more or less, contemporary. Nevertheless, the plots of both Homecoming and Maniac, as well as series 4 of Poldark, which I have just completed watching, all involve or revolve around the inappropriate use of drugs prescribed by unethical doctors. This can hardly be a coincidence.
Indeed, at the same time, an essay appeared in the Sunday New York Times book review by the author Jonathan Lethem, commenting on the use of drugs, many of them fictitious, as plot devices in contemporary literature. A good example of this would be “My Year of Rest and Relaxation, “ a recent rather hilarious novel by Ottessa Moshfegh, which describes the antiheroine’s use of an extraordinary number of drugs, many in exotic combinations, as prescribed to her by a (morally dubious) psychiatrist. The use of drugs, especially fictitious drugs, is a good way of moving a plot forward because ,just like magic in previous centuries, they enable a character to do anything that the author wishes. So, what exactly are these drugs, if they really exist, or what might they be, if they are fictitious? Here I will deal with Homecoming and next month I will deal with Poldark.
One thing we should note is that the use of drugs or bizarre medical techniques employed by evil doctors for nefarious purposes is nothing new in the history of literature. One can go back to 1836 when George Buchner wrote (but never completed) his play Woyzeck, later to be made into the famous Alban Berg opera, Wozzeck. Here a character known only as “The Doctor” uses the hapless Woyzeck as a research subject without caring a jot about what happens to him. The Doctor’s experiment involves forcing Woyzeck to eat nothing but peas for weeks on end – something that eventually drives him completely insane. Closer to our own time one could do no better than take note of the awful Dr. Benway in William Burroughs “Naked Lunch.” Like Buchner’s doctor, Dr. Benway is extremely cavalier (to say the least) in his treatment of patients and the drugs he gives them. Here, for example, is Dr. Benway operating in an auditorium filled with observing medical students:
“Now, boys, you won’t see this operation performed very often and there’s a reason for that … You see it has absolutely no medical value. No one knows what the purpose of it originally was or if it had a purpose at all. Personally I think it was a pure artistic creation from the beginning. Just as a bull fighter with his skill and knowledge extricates himself from danger he has himself invoked, so in this operation the surgeon deliberately endangers his patient, and then, with incredible speed and celerity, rescues him from death at the last possible split second …Did any of you ever see Doctor Tetrazzini perform? I say perform advisedly because his operations were performances. He would start by throwing a scalpel across the room into the patient and then make his entrance like a ballet dancer. His speed was incredible: `I don’t give them time to die,’ he would say. Tumors put him in a frenzy of rage. `Fucking undisciplined cells!’ he would snarl, advancing on the tumor like a knife-fighter.”
When asked why he wrote “Naked Lunch,” Burroughs replied that he wanted to “destroy all forms of rational thought” – and he certainly went a long way towards doing just that. In the satirical tradition of Jonathan Swift, the doctors conjured up by Buchner, Burroughs and others are reflections of an uncaring world that has gone completely insane and no longer makes any sense whatsoever. Indeed, it is sometimes difficult to actually determine what is fact and what is fiction. Do individuals like Dr. Benway actually exist in the real world? Homecoming would like to convince us that they do and, what is more, that they are operating at the behest of our own government, something that is potentially easier to believe these days.
A really good example of this kind of thing is the “secret” operation run by the CIA in the mid 1950s to mid 1960s known as MK-ULTRA, a program devoted to discovering new kinds of drugs or other procedures that could be used to incapacitate or influence the enemies of the United States, primarily “Communists.” There is actually very good evidence that the CIA did use doctors to conduct experiments using drugs designed to “brainwash” people, something that they believed was being done by their Communist adversaries (as illustrated, for example, in the movie the Manchurian Candidate). It is now quite clear that the CIA experimented with LSD, mescaline and Buzz (3-Quinuclidiny benzilate), often on unknowing victims, and sometimes with devastating effects. Some stories surrounding this have become quite well known, such as the alleged role of the CIA in the “suicide” of Frank Olson who threw himself out of a New York hotel window – a story recently expertly recounted in the miniseries Wormwood. We know that operations mounted by MK-ULTRA also influenced people like the writer Ken Kesey as recounted in Tom Woolf’s classic account, “The Electric Kool Aid Acid Test.” The fact that things like this really did happen makes it easier to appreciate the use of paranoid fantasies in literature and drama – perhaps they aren’t so crazy after all?
Which brings us back to Homecoming. If you haven’t seen it, and you certainly should, I will recount some of the story, but I can’t guarantee an absence of spoilers, sorry! The story centers on Heidi Bergman, a caseworker at the ‘Homecoming Transitional Support Centre,’ a special purpose live-in facility run by the Geist Group, a shadowy corporation who are only in it for the money. The purpose of the facility is ostensibly to help soldiers transition back to civilian life. Most of the inmates suffer from post-traumatic stress disorder (PTSD) and are being treated with a novel drug which is supposed to be able to “cure” them by erasing the toxic memories associated with their combat experiences. In actuality, the corporation hopes that use of their drug will result in soldiers who cannot remember their traumatic experiences and can therefore be redeployed into the war arena, which would be much cheaper than having to train new soldiers. The Geist Group hope to profit from their success in treating soldiers by convincing the military to invest in their operation. As things turn out, the drug that the soldiers receive does more than just erase toxic PTSD-linked memories. It erases all of their memories, resulting in a type of retrograde amnesia. The effects are clearly dose-dependent, and when the normal dose is doubled, as observed by Heidi when treating a patient with whom she has formed a romantic connection, the patient becomes virtually catatonic. Ultimately Heidi treats herself with the drug and much of the plot revolves around her recovering from her amnesia and rediscovering what happened at the facility and, ultimately who was responsible for what was going on and why. Although the story presented is presumably fiction, it is interesting to speculate about the nature of the drug used. Could such a drug possibly exist? Are there any clues provided that might allow us to identify what it might be? Here is what we ‘know.’ The drug is a natural product. As shown in one of the episodes it is derived from a plant, which looks a little like a type of bromeliad, but isn’t identified. As indicated from the writing on packages used for distributing the drug, the plant grows in Vietnam. I think that the implication here is that the properties of the plant have been discovered as the result of an Asian medical folk tradition. Indeed, this is quite a common way of discovering new drugs. For example, the drug reserpine, which has profound effects on mood and the cardiovascular system owing to its actions on biogenic amine storage in nerve terminals, is derived from the plant Rauwolfia serpentina and was introduced into western medicine as a result of its prior use in Indian folk medicine. Similarly, artemisinin, currently the most effective drug for the treatment of malaria, was derived from the sweet wormwood plant used in traditional Chinese medicine. And there are many other examples of this kind of thing throughout history including the discovery of aspirin, digoxin and quinine.
The plant employed in Homecoming contains red berries. The berries are removed from the plant and dried. They are then extracted to produce a red liquid. This liquid is what is then used to treat the patients in the Homecoming facility by introducing it into their food, which is served in a special cafeteria where nobody else is permitted to eat. The red liquid doesn’t seem to be further processed in any way, so we have no idea about the active chemical principles involved in its action. It is quite possible that the red liquid contains more than one active component. This is certainly the case with many crude natural remedies. Recall that crude opium, for example, contains both morphine and codeine as well as a variety of other active non opioid components. A second piece of information concerning the nature of the Homecoming drug is that it produces retrograde amnesia. The drug is administered over a period of several weeks, suggesting a cumulative effect. It is also implied that increasing doses are used over time and (spoiler alert!) Heidi’s amnesia is produced by a single dose of the drug which she receives by eating in the patients’ cafeteria at an advanced stage of the drug-titrating proceedings.
It seems as though the Geist Group has done some research on the mechanism of action of their drug. At some point the group’s major protagonist in the story, a man named Colin, gives a lecture to the military about successes the company have had when treating their patients. One cannot really see his Power Point slides except in one instance where the structure of the neurotransmitter dopamine is clearly displayed. Presumably, the company has discovered that dopamine is somehow involved in the action of the drug. Two other clues are also provided. One of the victims of drug treatment at the Homecoming establishment gives a government investigator a leaf of an unidentified plant, presumably as a clue to what is going on and to help him with his investigation. Another scene takes place in a room where a picture of a leaf is displayed on one wall with the word ‘Manchineel’ next to it.
So, what are we to make of all of this? What could the drug used in Homecoming be and how could it produce its effects? PTSD is viewed as a topic of great importance these days, and is the subject of a lot of cutting edge research. Fear responses, which consist of rapid cognitive, motor and sympathetic components, are normally important reactions to stimuli that that indicate impending danger and are typically triggered in warfare or in situations associated with habitual abuse. These responses occur rapidly but then quickly disappear once the danger is passed, something that is essential for animals to be able to respond efficiently in the future. However, failure to extinguish fear response memories is a key contributing factor in anxiety and stress-related disorders such as PTSD, in which fear and panic are triggered by cues incorrectly associated with actual danger.
In order to treat such disorders, it is important to effectively ‘extinguish’ (a term from classical conditioning) maladaptive physical responses to past trauma, while reducing and processing the negative “valence” (emotional response and interpretation) associated with the memory. How can this be achieved? One thing we know is that various forms of therapy (Cognitive Behavioral Therapy, Interpersonal therapy, and Eye Movement Desensitization and Reprocessing techniques) are often helpful. In addition, some drugs have also been found to have beneficial effects, and more so in combination with talk therapies. These drugs are typically SSRIs such as Zoloft and SNRIs such as Cymbalta. However, given the fact that these drugs don’t always work very well, current research attempts to produce better pharmacological agents whose actions are based on a clear understanding of the cellular and molecular processes underlying PTSD.
Like all learning and memory phenomena, “fear extinction” is dependent on specific neuronal circuits in the brain, which are regulated by neurotransmitter molecules and their receptors. Several key brain areas including the amygdala (AMY), hippocampus (HPC), medial prefrontal cortex (mPFC), periaqueductal gray (PAG), bed nucleus of the stria terminalis, and others have been implicated in fear extinction. What kinds of drugs might therefore be expected to act on these circuits and thereby enable fear extinction? According to Professor Jelena Radulovic of Northwestern University in Chicago (https://www.scholars.northwestern.edu/en/persons/jelena-radulovic), a world expert on the use of drugs for PTSD in animal research, “there is a general agreement that fear extinction is based on learning that cues and situations associated with past stressful events no longer predict such outcomes.” One well established fact about learning and memory is that it involves what is known as “synaptic plasticity,” a phenomenon during which the strength of neurotransmission at particular synapses is either strengthened or reduced for long periods of time. We know that this type of synaptic plasticity is usually regulated by the neurotransmitter glutamate through its action on glutamate receptors. In particular, one type of glutamate receptor known as an N-methyl-D-aspartic acid (NMDA) receptor is clearly important for synaptic signaling in connection with memory. Hence, as demonstrated by Professor Radulovic and her colleagues, drugs that act on NMDA receptors might be helpful for the treatment of PTSD. In particular, drugs that activate NMDA receptors may be useful in these situations. However, when considering NMDA receptors as a therapeutic option, one must be very careful as we also know that activating these receptors too intensely can be counter-productive and produce the death of nerve cells, resulting in long term memory deficits, seizures and other symptoms.
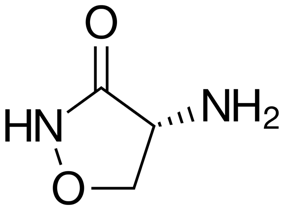
Do substances that can activate NMDA receptors exist in plants? Plants often contain what are called “D” amino acids. These are amino acids that have an unusual stereochemistry and are different in this respect from the amino acids that are normally found in proteins. It is known that some of these, such as D-serine or D-alanine analogue D-cycloserine can activate NMDA receptors. Moreover, their mechanism of action and the receptor activation they produce is fairly gentle compared to more powerful drugs. Hence, it is a fairly reasonable hypothesis that something along these lines is to be found in the red liquid.
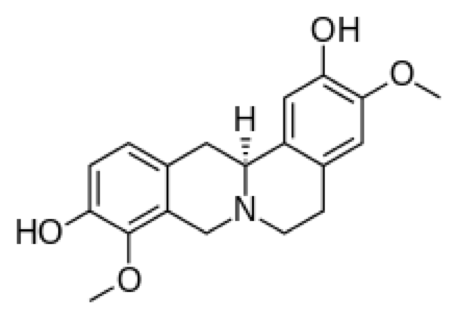
What about the neurotransmitter dopamine? Here again, there is every reason to believe that dopaminergic mechanisms are also involved in the pathogenesis of PTSD. There is convincing research suggesting that activation of dopamine receptors may also be helpful in fear extinction. Certain neurons that use dopamine as a neurotransmitter (they are known as ventral tegmental neurons, VTA) innervate both the amygdala and medial prefrontal cortex. VTA neurons play a key role in the determination of observed valence associated with different behaviors in animal models. Indeed, preclinical data has shown that drugs that activate some types of dopamine receptors are helpful in treating models of PTSD in rodents. As far as natural products are concerned, there are a good number of naturally occurring dopamine receptor agonists. Just as an example from the recent literature, one might consider the molecule l-stepholidine, which can be obtained from the plants of the genus Stephania, such as Stephania intermedia which is found growing in southeast Asia and has been widely used in traditional Asian medicine. This molecule has diverse effects on dopamine receptors – it activates some types and inhibits others and, among other things, appears to be useful in the treatment of drug addiction.
What about the word ‘Manchineel’ written on the wall of the office? I think this is a red herring. All the departments at the Geist companies are named after trees of one sort or another. On the other hand the manchineel tree is certainly highly toxic, containing a number of extremely irritant substances. Just touching it can produce severe contact dermatitis and if you happen to eat one ……..well, just don’t…. that’s all. It is unlikely that any extract of this or a related plant would be useful for treating PTSD. Indeed, the experience of eating what the Guinness Book of World Records calls the “most poisonous plant in the world” is more likely to induce PTSD rather than cure it.
So, what can we conclude? The identity of the plant that produces the red berries isn’t clear, but it seems to grow in southeast Asia. The drug appears to be a plant extract rather than a pure substance, meaning that it could contain more than one active component. Based on what we know about the molecular mechanisms that underlie PTSD, we might hypothesize that molecules that interact with NMDA and dopamine receptors could be involved. And there are natural product candidates that would seem to have the appropriate properties. However, any beneficial effects are likely to be critically dependent on dose and, as indicated in the program, higher doses can produce serious side effects. Much of this would be consistent with an NMDA receptor mediated mechanism of some type. Activation of what are known as D1 dopamine receptors can have the effect of enhancing the actions of drugs at NMDA receptors, making them more potent than they are in isolation. So, my tentative conclusion is the red liquid contains substances that produce their effects through joint activation of NMDA and dopamine (D1) receptors. Unfortunately, although the drug does appear to target memories, it is not specific enough to target PTSD associated memories in particular and so, even at a therapeutic dose, produces a more generalized form of retrograde amnesia. Of course, it is quite possible that the military and the Geist Corporation will decide that this profile of effects is appropriate for their ultimate goals of being able to recycle soldiers back into the combat arena. Indeed, it might be argued that they might actually make rather good soldiers. Such a conclusion of course ignores the ethical problems associated with their approach. But, in paranoid fantasies of this sort such dichotomies are always at the center of the action. We are horrified…but maybe we should just try to see things from the point of view of the CIA and the Corporation, surely a bunch of highly intelligent people. After all in the end it’s all about money and power isn’t it? Why can’t we see that?
Will there be a Homecoming 2? I don’t know but I would certainly love to see how these experiments in human psychopharmacology turn out in Cableland– one thing I can say, is that this type of experimentation is rarely approved by NIH research grants, but who knows what lurks in the deep pockets of these secret investors…?
FURTHER READING:
N-Methyl D-aspartate receptor subunit signaling in fear extinction. Radulovic J, Ren LY, Gao C. Psychopharmacology (Berl). 2018 Sep 20. doi: 10.1007/s00213-018-5022-5. [Epub ahead of print] Review. PMID:30238131
Pharmacology of cognitive enhancers for exposure-based therapy of fear, anxiety and trauma-related disorders. Singewald N, Schmuckermair C, Whittle N, Holmes A, Ressler KJ. Pharmacol Ther. 2015 May;149:150-90. doi: 10.1016/j.pharmthera.2014.12.004. Epub 2014 Dec 27. Review. PMID: 25550231
Dopamine D1-Like Receptor Agonist and D2-Like Receptor Antagonist (-)-Stepholidine Reduces Reinstatement of Drug-Seeking Behavior for 3,4-Methylenedioxypyrovalerone (MDPV) in Rats. Hicks C, Huang P, Ramos L, Nayak SU, Caro Y, Reitz AB, Smith GR, Lee DY, Rawls SM, Liu-Chen LY. ACS Chem Neurosci. 2018 Jun 20;9(6):1327-1337. doi: 10.1021/acschemneuro.7b00510. Epub 2018 Apr 6. PMID: 29597343
